Anticipating Your First Pelvic Exam and Pap Test
At our practice, where we integrate conventional and alternative ways of thinking, there has never been any doubt about the importance of annual examinations and regular Pap screenings for our patients. The anticipation of your first pelvic exam and Pap test can be nerve racking, but it doesn’t need to be. We know that knowledge is key, and by knowing more, women find they will worry less.
At marcellepick.com we want you to know what to expect during your routine Pap test and gynecologic exam. Has your clinician performed the Pap test without an explanation of what to expect and why it’s being done? That probably didn’t leave you feeling great. As women we need to ask the right questions and know and understand the importance of regular pelvic exams and Pap smears. We believe this information can help you become your own best advocate – when you comprehend why this is all needed, you can feel more comfortable with the procedure.
Both traditional and alternative practitioners advocate for an annual pelvic examination and Pap smear. Why? This standard of care has proven to be one of the best preventative combos there is to protect women’s health and longevity The Pap smear test was developed by, and named after, Dr. George Papanicolaou (1883–1962) for the purpose of early identification of cervical cancer. Soon after its introduction, the Pap smear proved effective at detecting precancerous lesions, which represent early — and still very treatable — indicators of cervical cancer risk.
Routine Pap Testing and Pelvic Exam: What Are They?
The Pap smear is an easy and reliable test and the procedure takes only minutes to perform. If you are approaching your first Pap smear and pelvic exam, relax; we will explain the procedure step by step.
First, you will be asked to disrobe from the waist down and put on a hospital gown. The clinician will ask you to sit at the edge of an exam table. Then, when instructed, you place your feet in the stirrup-style foot rests and lie back on the table (like the women in labor depicted on TV or movies). The clinician will ask you to separate your thighs and stay calm so the muscles are relaxed. The more relaxed and dropped apart your legs remain, the more comfortable you will be and the quicker the procedure will go. (If you wiggle your toes it is a great way to reduce tension in the legs, groin, or buttocks.) This position is often intimidating for women as they have their first pelvic exam but for many it gets better as time goes by.
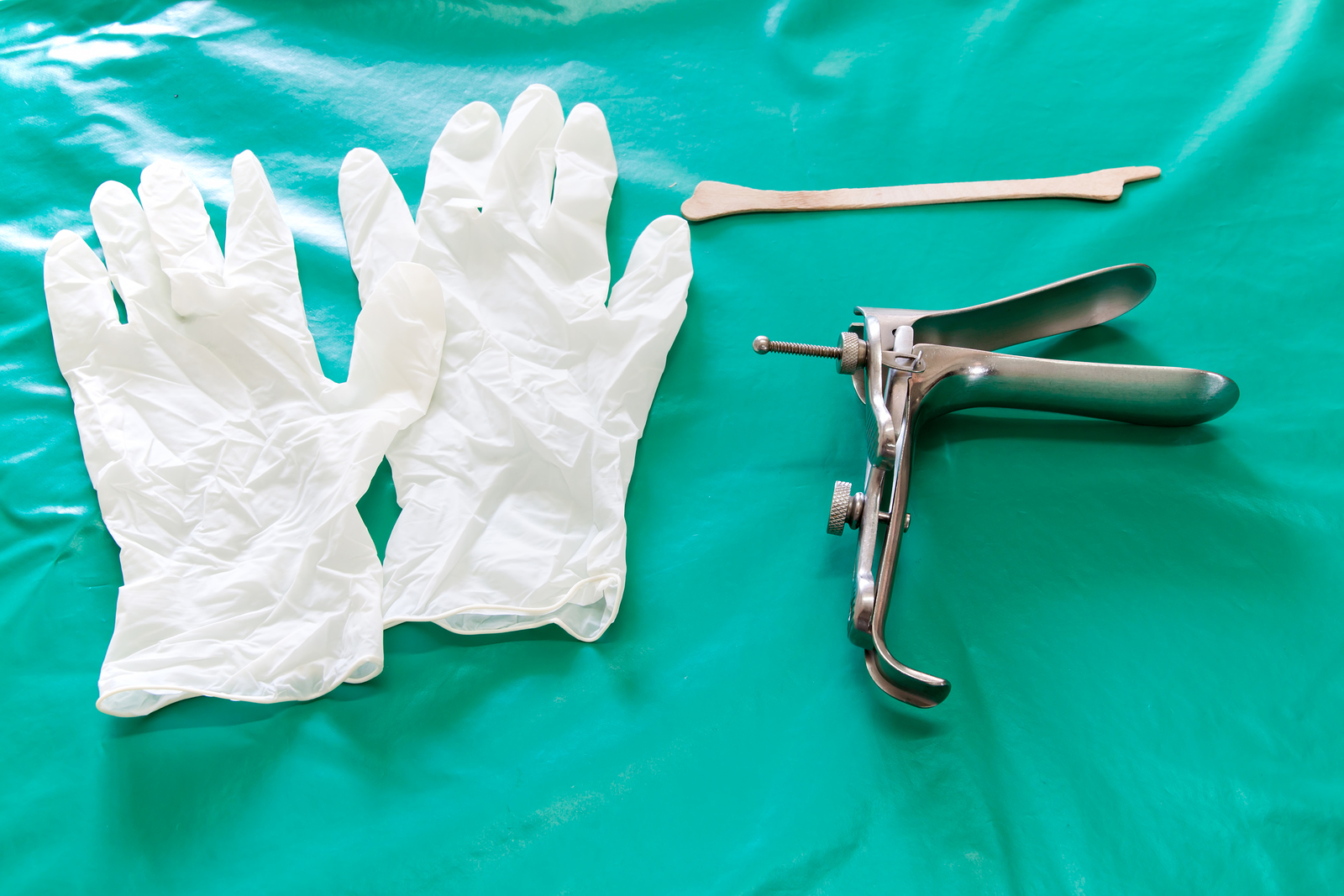
With a gloved hand the examiner will touch the exterior of the vulva to separate the labia and view the external genitalia for normalcy. To widen the opening a speculum, which is similar to a tampon applicator with a handle, is then gently inserted into the vagina. There are different sizes and styles of speculums used for different women. The speculum allows the clinician to view the vaginal walls and the cervix. The cervix is located high up in the vagina. It resembles a mini bagel projecting into the vagina, and if you were to touch it with your finger you will notice it feels like a firm, nose-like protrusion. The cervix is occasionally positioned so it is hard to see, but an experienced clinician can usually find it with a little gentle shifting of the speculum.
When the speculum is in place, the clinician will collect a sample of tissue from the exterior of the cervix (ectocervix) with a tool described as a spatula, then another from the cervical canal to the womb (endocervix) with a brush like instrument called a cytobrush. There are a number of devices which are used to gather samples, the most common being a contoured plastic spatula comparable to a tongue depressor. A little mascara-like brush is used to swish the interior of the cervical canal, and a small plastic broom-like brush is also often used. All these devices are gentle but can feel a bit odd to the patient when used. Some women have a very tender cervix and may experience more discomfort than others. If a woman has a more fragile cervix it may bleed a small amount when scraped, but this is only a temporary problem with no major side effects.
These days it is pretty customary for the clinician to place the collected samples in a liquid-based container, but in some clinics the samples are still smeared onto glass slides and a fixative applied. This is by far no longer the norm. Chlamydia and gonorrhea testing can now be done with the pap smear if is is collected using the ThinPrep methods (described below). If there are vaginal symptoms of concern, the clinician may use a Q-tip to swab the vaginal walls and then check the sample under a microscope for signs of a vaginal yeast infection or other types of infection.
The speculum is then removed; at this point the clinician typically performs a quick bimanual examination, where she or he feels the uterus and ovaries as is possible with their skillful hands — placing two fingers of one hand within the vagina and the other hand on the lower belly. Then the clinician will press gently to feel what cannot be seen.
The Pap sample is sent to a pathology lab for the technician to review the cells under a microscope, checking for normal and abnormal features. An HPV DNA analysis can also be done at that time if requested. Many patients are choosing to do this as there is such a high association with HPV positive paps and cervical changes that can need further evaluation. Many of these changes do not have any symptoms. When the analysis is complete a report is sent to the clinic.
The clinic usually sends you a written notice that the pap and other tests were normal or require more follow up. For more information, read our article about pap testing results. Various clinics have different policies, and might only contact you if the results are abnormal, so if you want to be notified of the results regardless of the results, be sure to ask them to do so.
The New ThinPrep Pap Smear — Liquid-based Technology
Originally, the Pap test consisted of using a small wooden spatula to sample the outermost cell layer of the cervical os (the opening to the uterus inside the vagina), then the sample was smeared onto a glass slide and a fixative solution was applied, then it was sent for further evaluation with a pathologist. (Hence the term Pap smear). Fortunately the technology and research has changed immensely over the past decade and a half. Now most Paps are liquid based and allow the practitioner to evaluate the cervix for abnormal changes, test for the human papillomavirus (HPV) DNA typing, and test for gonorrhea and chlamydia. The HPV/DNA typing assists greatly in the management of abnormal paps.
With the new “liquid-based” Pap tests (i.e., ThinPrep® and SurePath®), the cell sample is placed in a jar of liquid fixative for rinsing and then it is transported to the lab for further processing and review. This process provides a cleaner, much easier-to-read sample and has a notably lower margin of error. This has had dramatic results for women as they now have the opportunity to see changes early and can then make lifestyle changes which definitely help with abnormal pap smear management. If you do discover that you have been exposed to a high–risk HPV strain, don’t be alarmed — it just means that you will be best served by close monitoring and follow-up over time to ensure your lifelong cervical health. Most women have been exposed to HPV, but the most important thing to understand is that dietary, and lifestyle changes can make the biggest difference in turning around the HPV status.
At the Women to Women clinic, we suggest a Pap smear just about every year for routine screening of sexually-active adult women, and occasionally more often to follow any minor abnormal cells found on previous Pap smear tests. This is because women may change sexual partners; monogamous women can have partners who stray; and ultimately, everyone’s risk status can change over time. Changes in stress levels and immune response can also lead a previously normal–testing woman to suddenly test abnormal.
We view the Pap test as somewhat of a Geiger counter for your overall health — especially because we interpret the presence of abnormal cervical cells as a sign of weakened immune system function. The fact is that delayed testing can place women at greater risk, and could reduce the probability of detecting abnormal cell changes early — which is the key to preventing cervical cancer.
For more information, read our articles about Pap smears and HPV.
Additional resources for women:
- Our Bodies, Ourselves: A New Edition for a New Era (2005 edition), from the Boston’s Women’s Health Book Collective.
- Changing Bodies, Changing Lives: A Book for Teens on Sex and Relationships (expanded 3rd edition), by Ruth Bell.